VERTEBRAL AUGMENTATION PROCEDURES – (Kyphoplasty, Vetebroplasty)
Osteoporosis is a major health problem in postmenopausal women and elderly patients of both sexes. The morbid event in osteoporosis is often a spinal compression fracture. To illustrate the scope of the problem, an estimated 700,000 new vertebral compression fractures occur each year in the United States.
Spinal compression fractures are associated with considerable morbidity and pain. Traditional treatments often are unsatisfactory. Conservative management with analgesics, bed rest, and bracing is often ineffective, and extensive reconstructive spinal surgery is poorly tolerated by elderly debilitated patients. Recently, percutaneous techniques to augment the collapsed vertebral body were described, including vertebroplasty and kyphoplasty.
Vertebroplasty
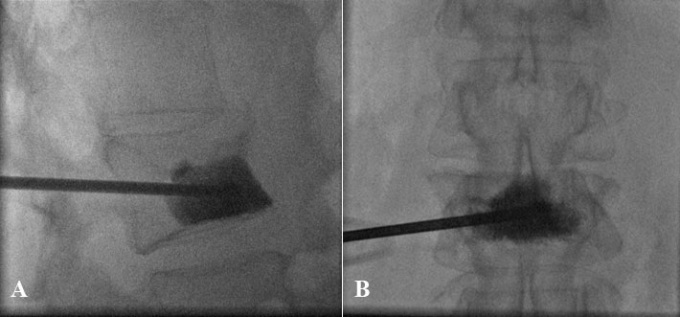
Vertebroplasty involves the injection of methylmethacrylate into the injured vertebral body via a needle, which is placed percutaneously using a transpedicular or extra-pedicular approach. High-quality fluoroscopic imaging is essential to ensure accurate needle placement and injection. The procedure can be done in a radiology suite or in an operating room with use of either conscious sedation or general anesthesia. Vertebroplasty provides pain relief by reinforcing the damaged vertebral body. Because the methylmethacrylate must be forced into the cancellous bone matrix, high injection pressures and an extremely liquid injectate are required, with potential for extravasation. The injection volume is usually 1 to 4 mL per side.
Kyphoplasty
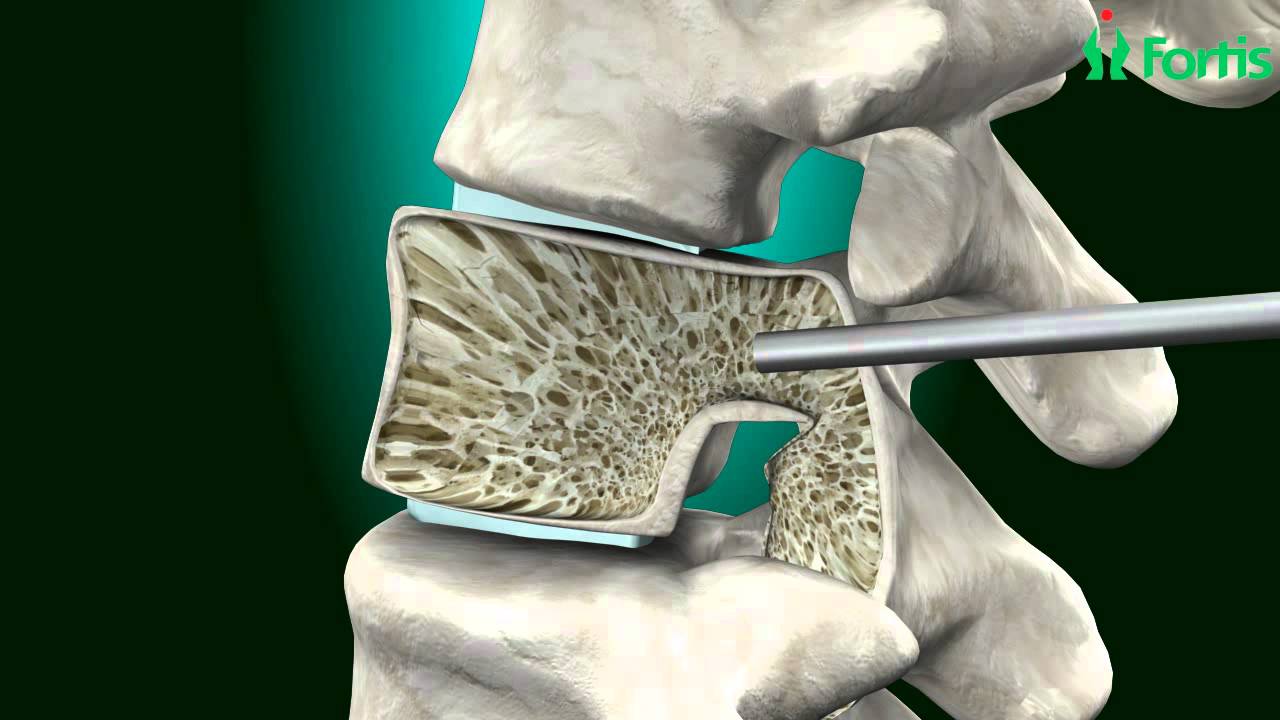
Kyphoplasty is a newer method of vertebral augmentation. A balloon placed inside the vertebral body is inflated to create a cavity, which is filled with methylmethacrylate using low-pressure injection. Similar to vertebroplasty, the procedure provides pain relief by restoring load-bearing capacity and stiffness of the injured vertebral body. In addition, balloon inflation has the capacity to reduce the fracture by restoring vertebral body height. Injection volume is usually 2 to 6 mL per side.
Both kyphoplasty and vertebroplasty are effective treatments of vertebral compression fractures. Garfin et al documented a 95% improvement in pain and considerable improvement in function after treatment with either technique. In addition, kyphoplasty was found to increase the height of the fractured vertebral body and decrease kyphosis by 50% if performed within 3 months of the injury.
Kyphoplasty may have a slight advantage through its potential to restore height of the vertebral body and to correct kyphosis caused by the fracture. Also, kyphoplasty appears to have a lower risk of extravasation because methylmethacrylate can be placed in a more viscous form via low-pressure injection, in contrast to vertebroplasty, which requires a more liquid injectate placed via high pressure injection.
These procedures are safe but not completely risk-free. A potential exists for spinal cord or nerve root compression due to extravasation of methylmethacrylate, pulmonary embolism from methylmethacrylate, and infection. The risk of refracture of a treated level appears to be low; however, the patient is still at risk for future vertebral compression fractures at other levels.
The most common indication for vertebral augmentation procedures is a benign osteoporotic compression fracture, but these techniques also can be used in selected patients with painful compression fractures secondary to multiple myeloma and metastatic tumors. The trend is toward early treatment of these fractures instead of trying weeks of often-futile conservative treatment. Early treatment provides faster pain relief and improved function and prevents prolonged periods of bed rest, which can lead to high morbidity in the elderly population.
أضف تعليقك